The criminal indictments of Donald Trump, we are told, ad nauseum, represent a “test,” indeed, a “stress test,” for American democracy. And it is a test, some claim, that we are failing. Really? Trump’s criminality has resulted in multiple criminal indictments for which he will stand trial and hopefully end up in prison. I tend to the position of Steve Benen, for whom Trump is a scandal-plagued politician in a country that has “all kinds of experience with scandal-plagued politicians getting indicted. It happens all the time. It doesn’t tear at the fabric of our civic lives. It does not open the door to political violence. It is, for lack of a better word, normal.”[1]
Well, not exactly normal. Trump is not only the first ex-president so indicted, but an ex-president whose toxicity has suffused the nation for six years. He is an ex-president who commands, via social media, an army of volatile extremists fully capable of mass violence on behalf of their leader, their very own Führer. My problem is that political commentators who dwell on Trump’s crusade to become an American autocrat by overturning a presidential election miss the bigger picture: the failed tests of democracy that litter American history. In what follows, I want to consider the Crimes of Trump in a different way. I want to take them as an opportunity to look anew at a few of the real failures of American democracy.
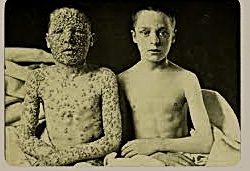
You want a “failure” of democracy? How about the widespread implementation of coercive sterilization that, beginning with Indiana’s eugenic sterilization law of 1907, robbed the nation’s undesirables – the “feebleminded,” the physically handicapped, the sexually “impure,” the chronically alcoholic, the wrong type of immigrants – of the right to procreate. Sterilization was the best way to prevent pollution of the gene pool of America’s Nordic white stock, and, in so doing, spare states the cost of maintaining future generations of defectives in publicly funded institutions.[2]
We should explore, among the nation’s most egregious failed tests, the unlawful and criminally abusive Indian private boarding schools that, from 1879 to 1969, embodied the federal government’s systematic effort to eradicate all aspects of ethnic identity among Native American children. In 408 schools in 37 states and territories,[3] Indian children as young as three were ripped away from their families and incarcerated in what were, in actuality, penal colonies funded by the Department of the Interior and run by the Catholic Church, especially the Jesuit orders. In “schools” built on unlawfully seized tribal lands, Indian children had tribal language, song, and tradition literally beaten out of them, sometimes to the point of death; suicide and death from drug use were common. The children’s unmarked graves in school basements and on school properties came to light in the 1990s; mass graveyards continue to be discovered to this day.[4]
And what of the 45,000 Native Americans, many products of the private boarding schools, who served in America’s military during the Second World War? Despite Congressional passage of the Indian Citizenship Act of 1924, postwar state legislatures, especially in the West, refused to comply. States like Utah, Arizona, New Mexico, and Maine strengthened “Jim Crow, Indian Style” to keep Indians, including veterans, away from the ballot box. Poll taxes, literacy tests, rejection of non-valid (i.e., reservation) mailing addresses, location of polling places far from tribal communities – such was the welcome afforded Indians who battled Hitler, Mussolini, and Hirohito in the name of representative democracy. Among the veterans were the Navajo Code Talkers, many from Arizona and New Mexico, whose service in the Pacific Theater was crucial to the successful island-hopping of the U.S. Marines. Only in 1957 did the Utah legislature grant Native Americans the vote. Even the Voting Rights Act of 1965 proved unavailing in Maine, which finally relented in 1967.
African Americans are no strangers to democracy’s unconscionable failures. Racism has seeped deep into the bone marrow of America, and the Civil War and its aftermath did little if anything to temper it. Need we mention the race laws that governed life in the Jim Crow South and provided an inspiring precedent for the Nazi lawyers who formulated the Nuremberg Laws of 1935 ? Consider the fate of the gallant African American soldiers who served in the Great War over a half century after the Civil War ended. The all-black 369th infantry regiment of New York, the legendary “Harlem Hellfighters,” had been unceremoniously assigned to the beleaguered French Army in March 1918. Under French command, the soldiers proved extraordinary combatants, and on December 13, 1918, the French government conferred its Croix de Guerre regimental citation on the 369th as well as individual Croix de Guerre medals on 171 regimental members.
But there was nothing of liberté, égalité, fraternité in their homecoming. During the Red Summer of 1919, race riots, often potentiated by the sight of black veterans in uniform, occurred in at least 26 cities. The sight of black troops in uniform was deeply threatening; local officials in Mississippi and Alabama had them strip naked on train platforms by way of jolting them back to second-class status; those who refused were severely beaten, sometimes to death. In 1919, of 83 recorded lynchings, 76 were of African Americans, of whom more than 11 were returning veterans.
Even Nazi “racial hygiene” of the 1930s failed to mitigate American racism. In the aftermath of Pearl Harbor, racist paranoia consumed the nation. How can we forget the 120,000 Japanese American citizens of coastal California subject to President Franklin Roosevelt’s Executive Order 9066 of February 19, 1942? These American citizens were forcibly relocated to one of ten concentration camps — euphemistically, “relocation” camps — throughout the western U.S. Their status as law-abiding citizens counted for nothing; their Japanese ancestry for everything. Businesses, homes, property, possessions – all were lost in this sterling example of American democracy in all its foundational impotence.
And what of African American male citizens who, in the wake of Pearl Harbor, sought to serve their country? African American recruits were denied enlistment in the Marine Corps and Army Air Corps. But they were welcomed into the U.S. Navy, as long as they were content to serve as mess attendants.
The U.S. Army was little better. In 1942 African Americans might enlist, but could only serve as replacement troops in the small number of all-black units. And what did they do? They were limited to construction and transport units that built the roads and landing strips that took white troops to theater of engagement. Sixty percent of the troops that built the 1,100-mile Ledo Road linking India and China were African Americans, as were one-third of those who built the 1,600-mile Alaska (aka Alcan) Highway that linked Alaska, Canada, and the continental United States. The latter project, begun three months after Pearl Harbor, took the black regiments to Alaska, where they began work in arctic temperatures that, one Veteran recounts, fell to -65F. African American troops spent nights in cloth tents, in which accumulated frost served as insulation. Their white counterparts were housed in Nissen huts and on army bases.[5]

An Army Corps Engineer at work on the Alaska Highway in early 1942.
Black troops in combat? No, not in 1942. Black combat pilots? Perish the thought. A war department report of 1920 declared African Americans lacked the intelligence, discipline, and courage to pilot aircraft. And then came the Tuskegee Experiment at the 66th Air Force Flying School in Tuskegee, Alabama – an experiment programmed to fail – and, following the forceful advocacy of Eleanor Roosevelt, the fabled Tuskegee Airmen.
_______________________
It’s 1924 and Albert Priddy, superintendent of the State Colony for Epileptics and Feebleminded outside Lynchburg, Virginia, has a problem. Like superintendents of institutions for mental, moral, and physical “defectives” that dot the country, Priddy selects those among his wards to be involuntarily sterilized in order to prevent them from passing their hereditary taint onto the next generation. Since his appointment in 1910, when the Colony opened, he has ordered the sterilization of more than 100 women, and his authority has been formalized in Virginia’s coercive sterilization law of 1924. Priddy himself helped draft the bill. According to the law, residents deemed “insane, idiotic, imbecilic, feeble-minded, or epileptic, and by the law of heredity probably potential parents of socially inadequate offspring likewise afflicted” should be sterilized within the institutions.[6]
Priddy’s problem is that he had recently been successfully sued by the husband of a female resident sterilized by his directive. To prevent any such eventuality in future, he now decides to personally engineer the legal appeal of one Carrie Buck, a young woman resident and the unwed mother of an infant daughter who lives with her in the Colony.
Carrie Buck is selected to “protest” her involuntary sterilization and to see it through the court system. But her odyssey through the courts – the County Court of Appeals, the Virginia Supreme Court, the U.S. Supreme Court – is sham, the outcome preordained in advance by those who have orchestrated her “appeal.” It is Priddy, in collaboration with a crony, State Senator Aubrey Strode, who has planned the ruse and then selected Buck’s “defense” attorney, charged with working for the young woman’s “acquittal.” In reality, the attorney, one Irving Whitehead, was a founding member of the Colony who sought the same judicial outcome as Priddy and Strode: Carrie Buck’s involuntary sterilization. Needless to say, he adduced no evidence at all on his “client’s” behalf.

Carrie and Emma Buck at the Virginia Colony in 1924, shortly before Carrie’s case went to trial.
So the constitutional legitimacy of Virginia’s coercive sterilization law was upheld, consecutively, by the Amherst Country Court of Appeals, the Virginia Supreme Court, and, finally, the U.S. Supreme Court. The Supreme Court found for the superintendent of the Virginia Colony in an 8-1 decision. Chief Justice William Howard Taft, an avowed proponent of coercive sterilization, assigned the majority decision to Associate Justice Oliver Wendell Holmes, another proponent of sterilization in the service of race betterment.
There was little, it turned out, to adjudicate. Eugenics of the time deemed feeble-mindedness a matter of heritable germ plasm, hence a family trait. It followed that assessment of individuals for coercive sterilization typically entailed investigation of family members. Buck’s mother, it turned out, was also “defective” and had resided in the Colony since 1920. Not only that, Buck’s infant daughter, Amelia, had been examined by the Colony physician and, so he swore in court, already showed signs of feeblemindedness. After breezily remarking that involuntary sterilization served public welfare no less than vaccination, Holmes ordered the sterilization of the allegedly imbecilic and sexually deviant Carrie Buck. “Three generations of imbecility are enough,” he concluded.[7]
After Buck, eugenic sterilization became lawful in the U.S., “fusing sterilization and eugenics in the public mind.”[8] But the case, we now know, manipulated the judicial system, and not in the interest of justice for the young woman about to lose her ability to procreate. In point of fact, Carrie Buck was far from feebleminded. She did well in grade school, earning special praise from her teachers for attendance and neat handwriting until her foster parents removed her from school after fifth grade. A feebleminded “moral delinquent” (Priddy’s words) destined to pass on defective genes to her progeny? Hardly. Buck’s pregnancy arose from rape by the nephew of her foster mother, Alice Dobbs. Fearing social embarrassment, the Dobbses petitioned Amherst County Court of Appeals to have Carrie incarcerated. The request was granted, and with the help of a complicit social worker, Carrie was packed up and deposited at the Lynchburg Colony. The social worker’s report of feeblemindedness and “moral delinquency” was all that Superintendent Priddy had to hear.
And Carrie’s infant daughter Vivian, characterized by the social worker as “not quite normal”? She died from pneumonia at age eight, but not before her name was added to her school’s honor roll. She never showed any signs of the “imbecility ” ascribed to her by Priddy in court.[9] (Hansen & King, 110-113, and elaborated by Lombroso). She was simply Carrie Buck’s daughter, and therefore part of the “deliberate plot carefully orchestrated by powerful institutional actors bent on winning constitutional authority to compulsory sterilization at any cost.”[10]
Buck v. Bell took place a decade after America’s arch-eugenicist, Harry Laughlin, administrator of the racist Eugenics Records Office at Cold Spring Harbor, Long Island, estimated that 15% of the American population, or 15 million people, would have to be sterilized to rid the U.S. of defective genetic stock. In 1924, the very year Buck v. Bell began its bogus journey through the court system, Congress passed the highly restrictive Immigration Law that remained on the books until 1965.[11] It followed by seven years the Immigration Act of 1917, which set in place the immigrant quota system while extending an immigrant’s eligibility period for deportation to five years. The Act was known as the “Asiatic Barred Zone Act,” since it barred Asians and other non-whites from immigrating. The Emergency Quota Act of 1921 restricted immigration from individual countries still further.
America is a nation of immigrants that has never warmed to immigrants. “Xenophobia,” the immigration scholar Erika Lee remarked a year ago, “powers the United States.”[12] Over the past 200 years, America has admitted over 80 million immigrants, all the while clinging to its irrational hostility to foreigners. Small wonder that Trump, the Prince of Xenophobes, himself the son and grandson of European immigrants, fired up his MAGA troops to keep immigrants away from these shores. Muslims found no safe harbor here, nor were asylum-seeking refugees from Central America welcome. In January 2017, Trump issued an executive order to construct a wall to keep Mexicans and South Americans, however desperate, from crossing the southern border.
What followed? Increasing numbers of immigrants were deported in record time; sanctuary cities became a thing of the past. The fragments of a wall never erected became a shrine to American nativism and exclusionism. Trump’s mother, who emigrated from Scotland in 1930, and his paternal grandfather, who emigrated from Germany in 1885, encountered no such wall, literally or figuratively, when they reached America.
For Trump himself, matters could have been different. The Immigration Law of 1917 stipulated among reasons for exclusion or subsequent deportation, “constitutional psychopathic inferiority.” Psychiatrists were available to make a determination of mental fitness. Consider this thought experiment: Imagine the ex-President of a South American dictatorship, El Presidente Donald Trump. A century ago, he seeks asylum in America following a popular uprising that repudiated his policies and sent him packing. But he is in the grips of an intractable narcissistic personality disorder so severe that he informs the interviewing psychiatrist that he is the Chosen One, destined to revitalize American greatness, and, given his mission, he cannot be subject to the American legal code.[13] It is doubtful he would have been permitted to disembark. That, at least, would have been a happy outcome of the Immigration Act of 1917.
_______________________
**I am grateful to my wife, Deane R. Stepansky, for suggesting the title of this essay. Her great love and support — not to mention her crack skills as Latinist, grammarian and proofreader — inform all the essays gathered in “Medicine, Health, and History.”
[1] Steve Benen, “Trump’s indictment creates a test our democracy can easily pass,” MaddowBlog, March 31, 2023 (https://www.msnbc.com/rachel-maddow-show/maddowblog/trumps-indictment-creates-test-democracy-can-easily-pass-rcna77553).
[2] American eugenicists like Madison Grant and Henry Stoddard proved an inspiration to German colleagues like Alfred Ploetz, the founder of Nazi racial “science.” Indeed, at the first International Congress for Eugenics in London in 1912, Ploetz proclaimed the U.S. a bold leader in the field of eugenics, foreshadowing the relationship between German and American eugenicists for whom the feebleminded, the physically handicapped, the criminals, alcoholics, and sexually “deviant” were all unworthy forms of life. Stefan Kühl, The Nazi Connection: Eugenics, American Racism, and German National Socialism (NY: OUP, 1994), ch 1, and more expansively and analytically, James Q. Whitman, Hitler’s American Model: The United States and the Making of Nazi Race Law (Princeton: Princeton Univ. Press, 2017). Whitman begins his book by noting that the transcript of the meeting among leading Nazi lawyers of June 5, 1934 – the meeting that outlined the three Nuremberg Laws of 1935 – reveals “detailed and lengthy discussions” of the race laws of the United States, especially the Jim Crow laws of the American South (pp. 1-5, 12-13, 29). American race law, the Nazis well understood, entailed far more than segregation; it encompassed immigration, citizenship (including requirements for naturalization), and anti-miscegenation laws (32ff.).
[3] The definitive source of facts and figures regarding the Indian private boarding schools is the Federal Indian Boarding School Initiative Investigative Report, released by the Department of the Interior on May 11, 2022. It is available in its entirety at https://www.bia.gov/sites/default/files/dup/inline-files/bsi_investigative_report_may_2022_508.pdf.
[4] Life in the private boarding schools is recounted by survivors and their descendants in two successive Reveal podcasts, “Buried Secrets: American Indian Boarding Schools,” Parts 1 & 2 released on March 18 and March 25, 2023. Both can be accessed at: https://revealnews.org/?s=Buried%20Secrets%3A%20. The podcasts focus on the Red Cloud Indian School of Lakota County, South Dakota. For an insightful overview of all the private boarding schools, see David W. Adams, Education for Extinction: American Indians and the Boarding School Experience, 1875-1928 (Norman: Univ. Press of Kansas, 1995) and Brendan J. Child, Boarding School Seasons: American Indian Families, 1900-1940 (Lincoln: Univ. of Nebraska Press, 1998), which makes extensive use of letters by students, parents, and school officials.
[5] From the recollections of Reginald Beverly, member of the 95th Engineering Regiment, one of the African American units that constructed the Alaska (Alcan) Highway in 1942, recorded in “African Americans in World War II: A Legacy of Patriotism and Valor” (1997), available at https://www.youtube.com/watch?v=vGpP3mj6FrU. For a readable overview of the experience of African American soldiers, including their experience in WWI, see Peter C. Baker, “The Tragic, Forgotten History of Black Military Veterans,” The New Yorker, November 27, 2016 (https://www.newyorker.com/news/news-desk/the-tragic-forgotten-history-of-black-military-veterans). General interest articles on the Harlem Hellfighters are plentiful on the internet; those interested in more scholarly historical presentations might begin with Stephen L. Harris & Rod Paschal, Harlem’s Hellfighters: The African-American 369th Infantry in World War I (Sterling, VA: Potomac Books, 2005).
[6] Randall Hansen & Desmond King, Sterilized by the State: Eugenics, Race, and the Population Scare in twentieth-Century North America (Cambridge: Cambridge University Press, 2013 ),104. All the histories of eugenics in America discuss Buck v. Bell. I have found Hansen & King the best chapter-length presentation. For those interested in a detailed, book-length account, there is Paul A. Lombardo, Three Generations, No Imbeciles: Eugenics, the Supreme Court, and Buck v. Bell (Baltimore: Johns Hopkins Univ. Press, 2008).
[7] Buck v. Bell, 274 U.S. 207 (1927).
[8] Molly Ladd-Taylor, Fixing the Poor: Eugenic Sterilization and Child Welfare in the Twentieth Century (Baltimore: Johns Hopkins Univ. Press, 2017), Introduction, and Hansen & King, op. cit., 110.
[9] Hansen & King, op. cit., 110-113, elaborated at length in Lombardo, op. cit.
[10] Hansen & King, op cit., 114.
[11] Ibid., 157, and, more expansively, in Henry Friedlander, The Origins of Nazi Genocide: From Euthanasia to the Final Solution (Chapel Hill: Univ. of North Carolina Press, 1995), ch 1.
[12] Erika Lee, “Xenophobia Powers the United States,” Public Books (https://www.publicbooks.org/xenophobia-powers-the-united-states), 6/15/2022.
[13] Trump is a textbook case of “narcissistic personality disorder” in the sense of Heinz Kohut, the founder of post-Freudian psychoanalytic self psychology. See Kohut, The Restoration of the Self (NY: IUP, 1977), and How Does Analysis Cure? edited by Arnold Goldberg, with the collaboration of Paul E. Stepansky (Chicago: University of Chicago Press, 1984). In this type of primitive pre-Oedipal pathology, the patient’s “grandiose self,” which requires a continuous stream of affirmation from others in the form, say, of mirroring or idealization, always masks a profound sense of inferiority. In Kohut’s lexicon, the grandiose self is “archaic” and, as such, brittle and prone to fragmentation. I discuss Kohut in my consideration of medical empathy in In the Hands of Doctors: Touch and Trust in Medical Care (Santa Barbara: Praeger, 2016; Keynote Books pbk, 2017), 55-59, 72-73.
Copyright © 2023 by Paul E. Stepansky. All rights reserved. The author kindly requests that educators using his blog essays in their courses and seminars let him know via info[at]keynote-books.com.